Ways to improve your thyroid and adrenal function
Ways to improve your thyroid and adrenal function
More than 12 percent of the population is likely to experience thyroid issues at some point in their lifetime—and sadly, this number is steadily rising, with the prevalence of hypothyroidism more than doubling in just the last three decades.
If you’re dealing with memory and concentration problems, brain fog, unexplained depression, anxiety, insomnia, fatigue, muscle loss, low libido, hair loss, constipation, dry skin, low blood pressure, low libido or struggling to lose weight, there’s a good chance it is caused by low thyroid function.
However, these are just common symptoms. Thyroid hormones are crucial for regulating metabolism, heart rate, blood pressure, vascular health and adrenal function. So, over time, an underactive thyroid (hypothyroidism) or overactive thyroid (hyperthyroidism) can wreak havoc on your whole system, leading to severe issues such as cognitive impairment, increased risk of heart attack and coronary artery disease, adrenal fatigue, and papillary thyroid cancer.
While women are most at risk for thyroid issues—largely due to declining estrogen and increased susceptibility to environmental stress—men are still vulnerable. Research suggests the prevalence of hypothyroidism ranges from 4 to 21 percent in women and 3 to 16 percent in men, varying by age group. That’s a lot of people walking around needlessly with FLC (Feel Like Crap Syndrome) that is 100% treatable.
Thyroid and adrenal issues also go hand-in-hand, and symptoms of adrenal fatigue can mirror those of hypothyroidism (e.g. insomnia, feeling “tired and wired,” palpitations, anxiety and fatigue), so it’s important to test thyroid and adrenal hormones together along with several other biomarkers to fully evaluate the health of these overlapping systems. When you are stressed your thyroid function declines.,
Testing thyroid, adrena and autoimmune function
Thyroid stimulating hormone
Thyroid stimulating hormone (TSH), which is made in the pituitary, regulates the production of the hormones triiodothyronine (T3) and thyroxine (T4) and signals the thyroid to release them into the bloodstream. As a result, elevated TSH levels can indicate hypothyroidism or an underactive thyroid, where the thyroid does not produce enough T3 and T4, prompting an increase in TSH to stimulate hormone production. Conversely, abnormally low TSH levels can indicate hyperthyroidism, or an overactive thyroid, where excessive T3 and T4 production results in reduced TSH secretion. Some doctors just check TSH if they suspect thyroid issues, not a full panel, which is needed to fully understand and treat low thyroid function.
Triiodothyronine and thyroxine
It is also not uncommon to have normal TSH levels but still have abnormal triiodothyronine (T3) and thyroxine (T4) levels, suggesting hypothyroidism or T3/T4 conversion issues. For this reason, it’s important to test free T3 and T4 levels in the blood to show the actual availability of these hormones for biological activity and provide a more comprehensive and nuanced assessment of thyroid function.
Thyroid peroxidase and anti-thyroglobulin antibodies
The presence of thyroid peroxidase (TPO) and anti-thyroglobulin antibodies (TgAb) can indicate an autoimmune reaction in which the immune system produces antibodies against thyroid proteins, potentially leading to thyroid damage and the decreased production of thyroid hormones. This is particularly helpful in diagnosing autoimmune thyroid diseases such as Graves’ and Hashimoto’s thyroiditis, which are responsible for 90 percent of hypothyroid cases. This is what I mentioned earlier—that 13 percent of our cohort of > 25,000 people have thyroid antibodies and a low-functioning thyroid, and most are not diagnosed.
Heavy metals
Environmental exposure to toxic materials such as aluminum (found in everyday household and personal care products), arsenic (found in seafood, wine, and groundwater), and mercury (found in fish, coal, plastics, pesticides, and certain dental fillings) can interfere with thyroid hormone production and impair adrenal gland function—leading to disrupted endocrine function and related autoimmune issues such as Hashimoto’s thyroiditis.
Addressing thyroid and adrenal dysfunction
Eliminate gluten and dairy. Gluten can trigger an autoimmune response in sensitive individuals, potentially leading to autoimmune thyroid conditions such as Hashimoto’s thyroiditis and increased cortisol demand, which can strain the adrenal glands and contribute to adrenal fatigue. Similarly, dairy can provoke inflammation and insulin resistance, worsening autoimmune thyroid issues due to the cross-reactivity of antibodies and stressing the adrenal glands by requiring them to produce more cortisol to manage blood sugar.
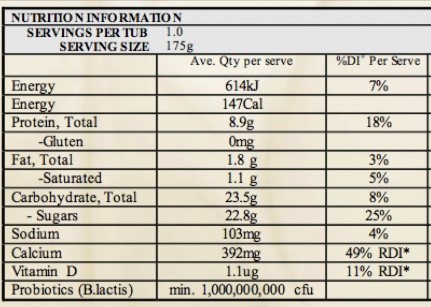
Support the gut. Because the gut-thyroid-adrenal axis is interconnected, eating probiotic foods and supplements that improve gut health, such as coconut yogurt, sauerkraut, and the probiotic strain saccharomyces boulardii can have positive effects on Hashimoto’s and adrenal function.
Cut caffeine intake. Caffeine stimulates cortisol production, which can overburden the adrenal glands, leading to adrenal fatigue and potentially exacerbating autoimmune conditions.
Eat a wide variety of healthy food to ensure you get the right vitamins and minerals. The thyroid depends on a number of nutrients to function optimally including iodine, zinc, selenium, vitamin D, and vitamins A and B. Vitamin C, B vitamins and magnesium all support adrenal function.
Stay away from starch and sugar. In addition to causing inflammation, insulin resistance, and being all around terrible for you, sugar and starch also cause elevated cortisol and adrenaline levels.
Ways to improve your thyroid and adrenal function Read More »